In This Post:
Presenters:

Katie Miller
Director of Consultant Relations

Kelly Guy
Head of Employer Partnerships
As we look at what’s happening out in the benefit space, it is clear that costs are constantly on the rise. U.S. employers are facing a difficult and expensive reality. But a lot of the contributing factors are ones that nutrition can actually positively influence. Things like obesity, diabetes, cardiovascular disease, and metabolic risk are really creating a conversation about nutrition that we haven’t always seen over time. The other thing happening at the same time is that employees are requesting coverage for GLP-1. They’re talking very adamantly with their medical providers about their interest in utilizing these medications. And we’re also hearing conversations about a desire for nutritional support, as well as support for gym memberships or discounts associated with gym memberships. And the conversation continues to evolve.
While organizations continue to invest in digital health tools, AI coaching apps, and point solutions that promise “personalization at scale,” finding the very best solution in the world often sounds the same. The conclusion is that it all comes down to engagement. Employers could have the very best solution in the world, but if it sits on the shelf and nobody uses it, it’s no use. It doesn’t add much value to the organization.
In honor of March 4 being World Obesity Day, we welcomed Kelly Guy, Head of Employer Partnerships at Nutrium, and Katie Miller, Director of Consultant Relations at Nutrium, to our webinar series to share how Nutrium supports this cause. Drawing on Kelly’s experience working with employers and benefits leaders, she outlined how organizations can improve employee well-being and reduce healthcare costs. They talked about AI, one of the hottest topics in healthcare, and how it can support healthcare initiatives and where it might be a little bit too much in the space.
About Nutrium
Nutrium Care provides personalized, high-touch nutrition care that scales globally and drives high engagement, with two-thirds of companies seeing adoption rates above 30%.
Nutrium’s clinically grounded care model adapts to individual needs, whether the focus is weight loss, chronic disease prevention, digestive health, or GLP-1 support, and is available in multiple languages and time zones.
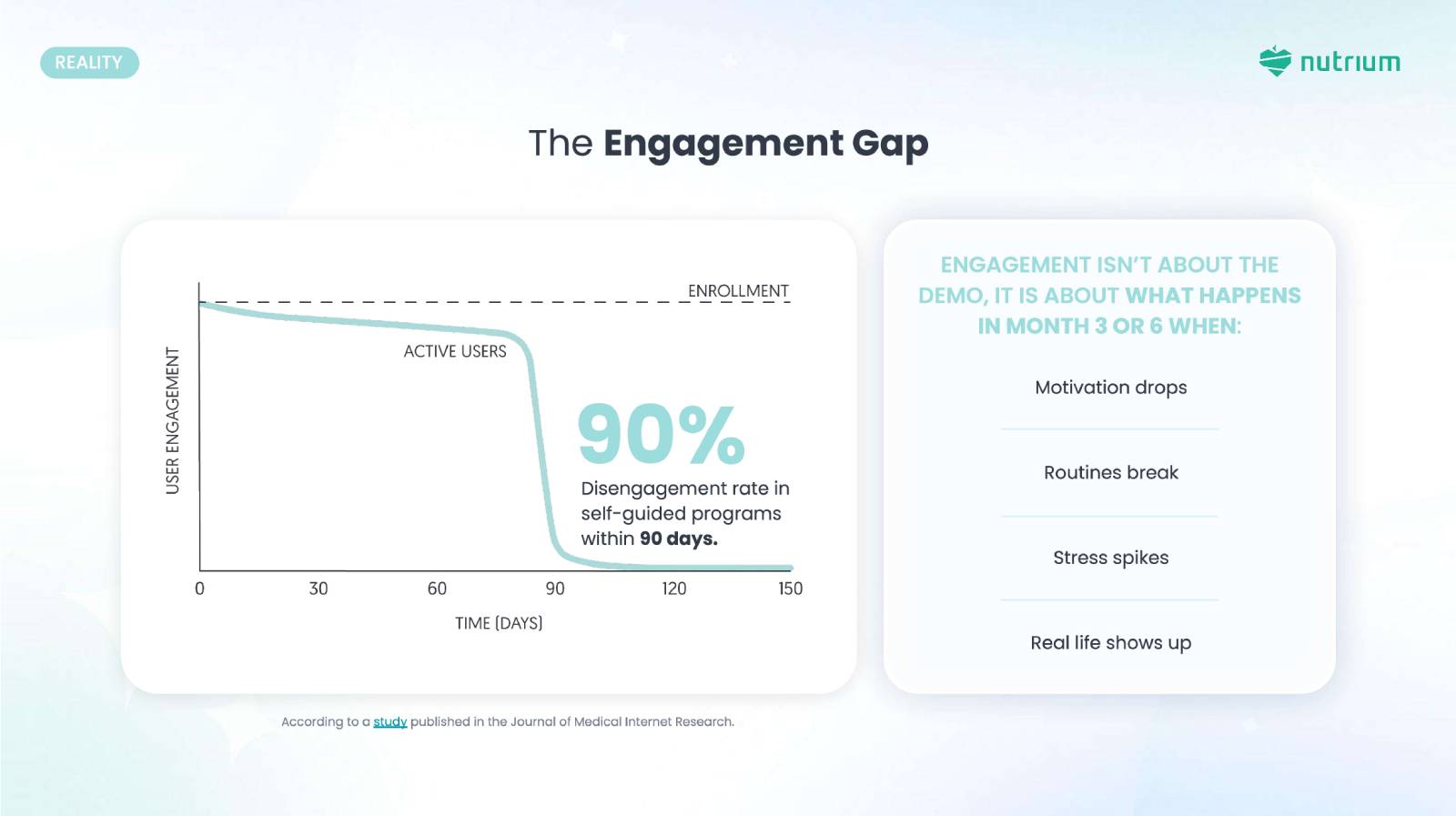
The Engagement Gap: Why Technology Alone Isn’t Enough
A lot of the different solutions share many similarities. A recent study actually showed that self-guided digital health programs experience disengagement rates as high as 90% within 90 days. And it really isn’t because employees don’t care or because the members aren’t dedicated enough to the process that they’re in. It comes down to the fact that life probably showed up something new they didn’t expect, something they didn’t plan for, or didn’t mention on the front end.
When that happens, personalization becomes more important, and that’s something Nutrium does through their dietetic support, and where dietitian-led care becomes a true differentiator.
By supporting employees early in their journey, Carrot helps prevent costly complications and ensures better long-term outcomes.
Here’s where digital tools with AI help:
- It can simplify food logging,
- track habits,
- surface patterns,
- answer low-risk questions,
- provide meal ideas, and
- help members stay organized between sessions.
One of Katie’s favourite examples of how AI was implemented at Nutrium is for meal logging. Something that was really tedious for her in the past and has made it hard for her to integrate it into day-to-day life is now part of it. By taking a photo of a meal, giving a quick voice recording about it, or even typing it out, Nutrium’s model will instantly analyse the meal’s ingredients and nutrients, so you and your dietitian can see them on the backend. And what that does is help reduce the time it takes to log as you go through the day, making it easier for people to integrate it into day-to-day life. And AI can also surface patterns really quickly.
What “Dietitian-Led” Really Means
The phrase “dietitian-led” is often used loosely in the market. In a truly clinician-centered model, registered dietitians (RDs) are central to the care journey from day one. Dietitians apply clinical judgment, manage medical history and metabolic risk, and continuously adapt plans as life circumstances change. They create accountability by owning the evolution of a member’s plan.
Rather than relying on members to re-engage when they feel stuck, clinicians proactively monitor progress and intervene early when risk appears.
A unified nutrition care model addresses the full health continuum within a single, coordinated experience. Instead of juggling disconnected programs, members receive structured intake, intentional matching with specialized dietitians, comprehensive clinical assessments, ongoing one-on-one appointments, and digital tracking tools that provide real-time visibility.
This structure allows care to evolve over time. As medications change, routines shift, or progress stalls, clinicians adapt strategies accordingly. Personalization is not limited to onboarding – it continues throughout the journey.

Measuring What Truly Matters
Employers often rely on surface-level engagement metrics: app logins, clicks, or content views. But meaningful progress requires deeper signals.
When vetting vendors, organizations should examine:
- Care Model Depth
- Follow-Up & Accountability
- Personalization Over Time
- Meaningful Progress Signals
- The Role of AI
When these checkpoints are satisfied, sustained engagement becomes more likely.
Why This Model Drives ROI
Long-term return on investment (ROI) in healthcare is driven by sustained behaviour change.
A model centered around licensed dietitians tends to produce:
- Higher sustained engagement
- Greater appointment adherence
- Clinically guided behavior change
- Reduced long-term risk exposure
When members return for follow-up appointments and maintain consistent relationships with clinicians, progress compounds. Behavior change becomes durable rather than temporary.
For employers, this translates into improved weight outcomes, better metabolic control, reduced complications, and ultimately, lower long-term healthcare costs.

Global and Cultural Responsiveness
In global workforces, culturally responsive care is essential. Nutrition is deeply tied to culture, tradition, language, and identity. A one-size-fits-all meal plan rarely resonates across diverse populations.
Models that match members with dietitians based on cultural fit, language fluency, and clinical specialization foster trust from the start. Structured intake processes that go beyond surface-level quizzes capture routines, preferences, clinical context, and readiness for change.
When members feel understood – not standardized – engagement increases.
Get in touch with Nutrium today!
Engagement is not about how exciting the demo looks during vendor selection. When evaluating vendors, employers should ask a simple but critical question: Is AI being used to enhance clinical care, or to substitute for it?
When these roles are clearly defined, outcomes improve.
AI reduces friction.
Humans drive personalization.
Outcomes require both.
When licensed dietitians lead care, supported by intelligent technology, engagement lasts longer, outcomes improve, and ROI becomes measurable.
For more information, contact:
Kelly Guy – kellyguy@nutrium.com
Katie Miller – katiemiller@nutrium.com
In case you missed it: Log in to access the full Meet A Vendor Presentation!
Not a subscriber? Request access.
Did you find this article interesting?
Don’t keep this knowledge to yourself – share it on your social media channels and spark engaging conversations!
